NAFLD and Dietary Patterns
Geographic regions with high prevalence of nonalcoholic steatohepatitis-related hepatic fibrosis are also observed to demonstrate high prevalence of metabolic disease risk factors and low consumption of fruits and vegetables
Nonalcoholic fatty liver disease (NAFLD) is the leading cause of chronic liver disease globally. We aim to evaluate prevalence and predictors of hepatic fibrosis among NAFLD patients, focusing on metabolic co-morbidities and dietary patterns.
Methods:
Quest Diagnostics laboratory data from 2017 to 2018 were used to identify NAFLD patients using a stepwise algorithm based on laboratory data and ICD-9/10 codes. Prevalence of fibrosis was assessed using a step-wise AST to platelet ratio index (APRI) algorithm. Multivariate logistic regression evaluated predictors of F2 fibrosis or cirrhosis. Prevalence of fibrosis was stratified by U.S. Department of Health and Human Services geographic regions and compared with region-specific data on metabolic diseases and dietary patterns (fruit and vegetable intake) using 2017 Behavioral Risk Factor Surveillance System.
Results:
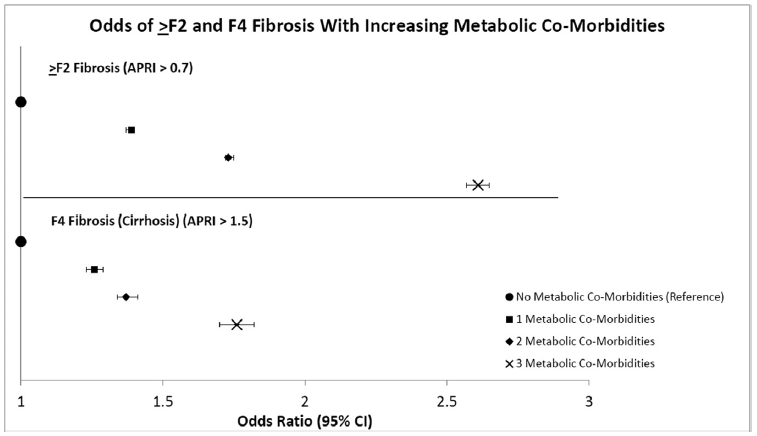
Among NAFLD patients, proportion of patients with APRI >2.0 was 1.58%, increasing to 3.05% (APRI > 1.5), 6.81% (APRI > 1.0), 12.67% (APRI > 0.7), and 21.87% with APRI >0.5. Increasing metabolic co-morbidities was associated with higher odds of fibrosis. Compared to patients with no metabolic co-morbidities, odds of >F2 fibrosis was OR 2.61 (95% CI 2.57e2.65, p < 0.01) and odds of cirrhosis was OR 1.76 (95% CI 1.70e1.82, p < 0.01) in patients with three metabolic co-morbidities. We observed that geographic regions with low fruit and vegetable intake and high prevalence of concurrent metabolic abnormalities to have the highest prevalence of NAFLD hepatic fibrosis.
Conclusion:
Increasing number of metabolic co-morbidities is associated with incremental increasing risk of hepatic fibrosis in NAFLD patients. We also observed patterns of low fruit and vegetable intake in regions with high prevalence of hepatic fibrosis.

